New Press Fellows arrive at Wolfson

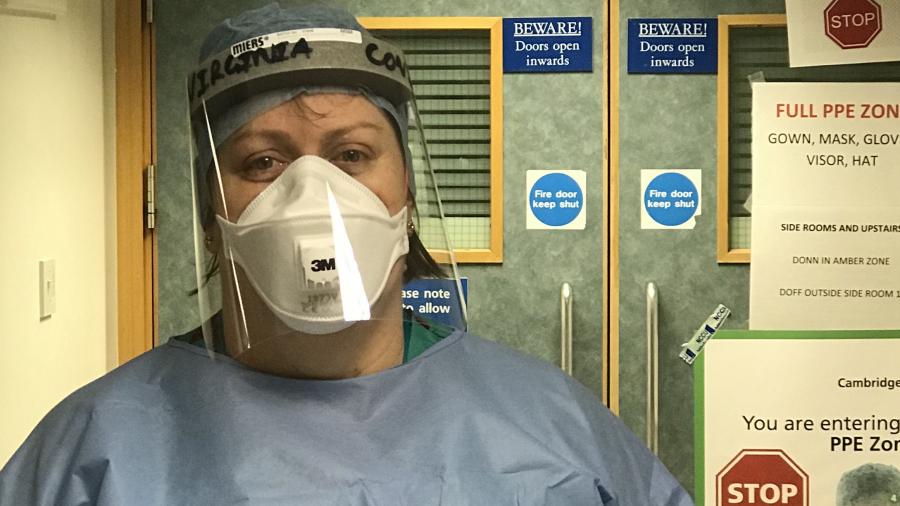
Wolfson Fellow Dr Virginia Newcombe is an Intensive Care Medicine and Emergency Physician currently working at Addenbrooke's ICU, and a Clinician Scientist in the Department of Medicine.

As a critical care physician, Dr Virginia Newcombe has seen her work environment at Addenbrooke's Hospital change completely over the past month. Capacity has more than doubled, including the opening of a new Intensive Care Unit. Drive-through testing for health care workers is taking place in the car park. Doctors and nurses are getting used to looking after patients in full PPE. And, of course, all the medical personnel are dealing with a new disease that presents many unknowns.
But she is nothing if not prepared. Virginia trained in medicine in Queensland in Australia and then came to the UK to complete a Masters in Epidemiology and a PhD in Neuroimaging and Traumatic Brain Injury. She has an active research programme, and works as a practicing physician. How does she balance the clinical and research aspects of her work?
"For me, as a clinician, it's very important to do research because otherwise you don't know the right questions to ask when you see patients," she says. At the moment Virginia is working entirely in intensive care, although "when there isn't a pandemic", she also works in Emergency Medicine.
The majority of patients in Addenbrooke's newly expanded ICU have COVID-19, but Virginia says the rate of admission for the disease has started to slow. The hospital's capacity to handle the pandemic has been good. And she says that her colleagues are generally coping well, for two reasons.
"First, the British are really quite good when there's something that needs to be done just 'getting on and doing it' without too much fuss. And second, I work in intensive care, which is a specialty that was born out of a pandemic. So if you work in the ICU and you're not willing to work in a pandemic then that's not the specialty for you."
Virginia is referring to the polio epidemic of the 1950s, when patients who could no longer breathe for themselves had to be put into negative-pressure 'iron lungs' (the current procedure is to use positive-pressure ventilators). This was the beginning of people being hooked up to machines that kept them alive and hence the birth of intensive care.
"One of the best things about the past few weeks is the fantastic team I have been working with—the cleaners, porters, health care assistants, nursing staff, radiographers, physios, doctors and all the others all have been doing their jobs with a smile and made it enjoyable to work despite the challenges."
Did she think that a pandemic was inevitable? "It's always been the great fear. We had warnings of the potential with H1N1 and SARS and if you look back through history, pandemics are not a new or unusual thing. The big question was when it would occur and how bad it would be."
But she notes that this pandemic is different, in that it seems to be disproportionately affecting older people around the world and that is true of the patients that Virginia is treating. "Usually pandemics affect the very young and the very old. Some, like SARS, affect those in the middle years. But fortunately with COVID-19 the vast majority of children don't seem to be getting sick. I'm not aware of there being any really ill children at the moment."
Virginia says the key to good care for the disease is to "do the simple things very well, and that means having fantastic nurses. The nurses are the ones who stay with the very ill patients for hours at a time, monitoring their condition, making sure that they don't develop complications from being in bed for a long time, and ensuring that all the interventions necessary for those on ventilators are carried out. There's also the other bits, like talking to families and so on."
It remains to be seen what the long-term consequences of those patients who have been on ventilators will be, she says. "Most COVID-19 patients need to be on a ventilator for two to three weeks. We know that a small number of patients who have been in the ICU for other reasons can develop Post-Intensive Care Syndrome, where they become more anxious than they were before, or may have some depression or cognitive issues. But we don't know if that will happen to COVID-19 patients."
Although COVID-19 presents much like respiratory diseases such as the flu, it does bring some unusual symptoms. One is the loss of smell and taste for some patients. Another is the likelihood that blood clots will form in the lungs.
"Anyone who is in bed for a long time is at risk of developing blood clots. The risk of patients with COVID-19 is far higher than normal and some patients get clots within the lungs themselves. But when patients come into hospital we give them medication to mitigate that risk."
Virginia credits the measures of lockdown and social distancing with flattening the peak of the disease. Does she think those measures should be lifted any time soon? "It's better in these things to plan for the worst and if you make all these plans and the worst doesn't happen, everyone thinks you overreacted but in fact you've done a very good job. So the NHS are planning for this to occur for a long time, months, if not one to two years."
One of the unknowns is whether having tested positive to the virus confers immunity to it. "This week, the WHO put out a statement saying that they don't know whether people can get it twice. Until there is widespread antibody testing the answer to that question won't be known. The advantage of a vaccine is that they tend to produce a higher immune response to very specific antibodies that tend to stay. So that's why a vaccine is going to be the most realistic way out of this. I'm hoping that the Oxford vaccine currently being trialled will prove to work very well."
Virginia has family in Australia, and she has also worked in the medical systems in the US and Canada. "One thing that's very clear is that having a health service that's nationalised is an advantage," she observes. "The NHS was able to mobilise a response very efficiently and maintain a high standard of care."
She says there is a concern amongst medics that people may not seek out medical care that they need during this time. She urges people who would seek medical treatment in normal conditions to go to A&E or contact their GP. "There is a concern that people are afraid to come to hospital in case they catch the virus. But there are areas in the hospital that are being kept as clean as possible so if people go there the risk will be minimised. A lot of GPs are doing online consultations as well."
We've seen photos on social media of the results of health care workers wearing PPE in hot conditions - the marks from the mask and so forth. Virginia says she's getting used to the new "normal" of looking after patients in full PPE, "I have to admit prior to this pandemic donning and doffing were words I thought only the poshest would use but now I use (and do) them many times in a shift. But it is much more difficult for the nurses, who have to stay with patients for hours at a time. As a doctor, I get to go in and out. But there is certainly no better feeling than removing my face mask to feel some fresh air on my face."







